Three Hospitals in the Third Trimester - Having a Baby in Cape Town, South Africa
When we first learned that we were pregnant, less than 2 months into our multi-year travels around the world, we had two options: 1) end our travels early and return home or 2) have our baby while we were traveling.
- GIVING BIRTH AT HOME -
Returning home would end our travels because, as full time travelers, we are exempt from paying for the mandatory U.S. medical insurance required by the Affordable Care Act - as long as we are outside of the country for at least 330 days out of the year (this was necessary prior to 2019). If we were to return at that time, we would not only have to pay for our airfare (roughly $1,250 each from where we would be when we needed to return), but we would also have to back-pay for that medical insurance as we would no longer be exempt. The penalty is either a flat amount assessed for each uninsured family member, or a percentage of your family income, whichever is greater. So, if we were to go back and NOT get insurance for ourselves, we would have to pay a penalty of $695 per adult, or 2.5% of household income - whichever was greater. For 2017, the maximum that could be charged was $3,625 per individual. If we wanted the insurance to help cover the birth of our child, we’d end up paying over $4,000 each - AND still end up with hospital and doctor bills totaling between $8,000-$16,000 for the birth (after insurance was applied). The truth is, in the United States, the hospital and physician costs for just about anything - especially childbirth - are so vague that you never really know what your bottom line will be (which led to the article “I tried to find out how much my son's birth would cost. No one would tell me” by Johnny Harris). The costs associated with going back would completely cripple our travel budget and require us to acquire new jobs once we returned - and that would be the end of our “endless travels”.
- GIVING BIRTH ABROAD -
Alternatively, we could give birth abroad - but our last trimester of pregnancy was already booked for South Africa in December, and a combination of Kenya, Tanzania, and Uganda in January and February. We did look into the hospitals in Nairobi, Kenya - but decided to change our plans and extend our stay in South Africa for the full third trimester (as we receive a 90-day travel visa there) and because we found an amazing Luxury Maternity Hospital that was going to cost a total of around $4,000 USD - and would provide us with the natural birth that we wanted. It was a fairly straightforward cost. You could choose a natural childbirth or a c-section and either had a slightly higher cost if there were complications. Very simple! So, near the beginning of our second trimester, we contacted that Hospital, filled out the paperwork, and were accepted by admissions. So, the decision was made and we changed our plans. We would be spending 3 months in Cape Town, South Africa!
[SPOILER: At 5 months old, we have still spent less than $4,000 USD on ALL expenses related to our baby so far - including hospital, doctors, midwives, vaccinations, travel gear, diapers, wipes, bum cream, etc. - so, IT IS WORTH IT TO HAVE YOUR BABY ABROAD!]
*** As US Citizens, our Visa-on-Arrival was 90 days long. Thus, we arranged to arrive roughly around the 7th month of pregnancy. Some airlines require a medical note to fly at 7-months, but it was not an issue for Jenny as she wasn’t showing much at that time and wasn’t having any complications. While we were waiting around for the baby to get ready, we found time to do a number of day tours in Cape Town and go on a Garden Route Tour as well as a couple Private Game Reserve Safari’s! It was an amazing adventure!
HOSPITAL #1
Here are images from the Origin Maternity Hospital’s website which convinced us to make this decision:
However, all of that changed in the first month of our third trimester - the middle of November - as we were sitting at our Airbnb in Madinaty, a suburb of Cairo in Egypt, and we saw a post on Facebook from Origin stating that they would be closing their doors on December 31st and that no births would occur there after that date. They notified us the next day, via email, that this was true and that we would need to find another hospital.
HOSPITAL #2
So, as our plans were already set and we couldn’t really change them again, we began our research to find the best hospitals in Cape Town - and we settled with Mediclinic Constantia - one of the highest rated hospitals in the area. A few weeks later we arrived in Cape Town and headed over to that hospital to take a look around and work with admissions to become accepted to birth at that hospital. The hospital looked fantastic as well! So, we were naturally quite pleased.
However - because we were already so far along - it was quite hard to find a doctor that would take us on as a client. As luck would have it, there was an OBGYN there with a new practice (only about 1-year thus far) that was available, so we signed up with her as we didn’t seem to have much of a choice.
When we had our first meeting with that OBGYN, she seemed very much for us wanting a natural birth. We did our exam and everything seemed alright. However, she was wary that Jenny was 37 years old and therefore wanted to avoid any delivery complications by not exceeding a 40 week pregnancy and noted that we would need to have an induction at 40 weeks if the baby hadn’t come by then. We were just at 31 weeks at this point, so it didn’t seem like it was too vital to think about it at that point.
Our next appointment was to be a month later. However, just a couple days prior to that appointment at 34 weeks +5 days, Jenny and I were changing Airbnb’s and decided to spend the intermediate time between check-out at one and check-in at the next by driving up to the top of Signal Hill and taking a few photos. When we arrived at the top, Jenny started feeling very nauseated and uncomfortable. Her skin started to get clammy and cold and she was beginning to pass out. So, I called the Hospital’s Emergency line and started driving toward the Hospital. They asked a few questions and as we descended from Signal Hill, Jenny began to feel better. The phone conversation ended in them recommending that she take a particular kind of pain reliever that we could find at the pharmacy. We did that and relaxed for the rest of the day.
At 35 weeks +2 days, we had our second appointment with the OBGYN. She was not happy to hear about the incident a few days earlier (as the nurses hadn’t informed her of it), and thought the recommendations they gave to us were wrong - we “should have came in and gotten checked out” according to her. At this check-up, everything still appeared fine, but the baby seemed to be on the lower level of weight gain and she thus recommended that Jenny start drinking Mom2B shakes and prescribed her Iron supplements to reduce the effects of “low blood pressure”. She also stated that she would want to induce at week 39 instead of 40 due to the situation.
At 36 weeks +1 day, Jenny’s parents sent us a virtual book gift to read: Natural Childbirth the Bradley Way: Revised Edition (Kindle Edition)
by Susan McCutcheon, which we didn’t begin reading right away.
At 36 weeks +6 days, there was another low-blood pressure incident and because of the conversation we had with the OBGYN during our last meeting, we checked into the hospital to be checked out. Jenny was put onto an external CTG machine that wrapped around her waist and measured her contractions and the baby’s heart beat. Everything checked out just fine, but the OBGYN did “hard push” us into staying the night - “just in case” - at an exuberant cost. We ended up passing on the extra night.
Based on the situation, we decided to begin reading the “Natural Childbirth the Bradley Way” book that night - but we had only read a few parts prior to our third OBGYN appointment at 37 weeks +2 days. The parts that we read were about how medications end up causing situations in the body that result in needing to use tools, cutting, and can even lead to requiring emergency c-sections during the delivery process - so the booked didn’t recommended using them. We admittedly thought we should have read much more of the book before going to that appointment.
Sadly, in the third appointment, the OBGYN was not pleased with the baby’s abdominal circumference - meaning she believed he had nearly no fat in the abdominal area and was at the lower bound of 3%. She also did an “internal exam” which included a soft sweep around cervix, which caused a worrying amount of blood during the urination Jenny had after the appointment. Thirdly, the OBGYN asked us two questions very sternly: “why are you so set on having a natural birth?” and “why don’t you want to use an epidural, again?” and then said that she would still have an anesthesiologist on hand in case Jenny changed her mind. So, we were a bit concerned that the doctor was trying to lead us towards a c-section instead at this point.
However, what was most concerning was that this OBGYN sprung an ultimatum on us at the end of that meeting. We were to sign a consent form stating that “I hereby consent to the following procedure(s) during labour and vaginal delivery:” that included assisted delivery (suction), episiotomy (cutting of the vaginal area), repair of a 2nd, 3rd, or 4th degree tear in theatre, blood products, manual removal of placenta, epidural, and a Cesarean section delivery. We were concerned because we were completely against many of these things in any situation other than an emergency life-threatening situation. And, while it seemed that these would only be used in an emergency situation, it also seemed like she was looking for a reason to make it more likely to end in a c-section delivery.
We asked if we could review the form and bring it back to her and she said that we absolutely needed to sign it before we left the office or we would need to discontinue her services. That was a total shock! We simply didn’t think we could find another doctor, so she had us in a corner! I (Bradley) insisted that I could not knowingly sign any commitment papers of any kind without fully reading them over and understanding them.
She begrudgingly allowed us the night to look them over and sign the papers and send her copies of the completed forms the following morning - BUT, we definitely had to pay the R14,000 deposit (roughly $1,000) to secure her services that day (which we would have had to do either way). So, we made the deposit, made an appointment for 5 days later (OBGYN recommended), and then walked out of the office all stunned.
Through the night we read as much as we possibly could and still didn’t want to sign the paperwork. We both had nightmares that we were going to have to fight the doctor off of Jenny to prevent her from performing a c-section. We understood the need to perform any of the procedures during a life-threatening emergency, but we completely felt that this doctor was going to find a reason to make this birth a c-section birth (as nearly all of her deliveries ended up becoming). As we couldn’t find an alternate doctor, we begrudgingly signed the papers and sent them to her via email - however, we made sure to include a “Birth Preferences Document” with that email that specifically spelled out what we wanted and didn’t want as well as what would need to happen, and what permissions would need to be attained, to detour from that plan. We felt a little safer, so we decided to take the next day to relax. However, we continued reading the book. The more we read, the more uncomfortable we were with our situation.
MIDWIFERY + HOSPITAL #3
So, after a day of relaxing, and another night of nightmares, we finished the book and then decided to continue looking around for a new doctor. We happened upon a place at the last possible minute - at 38 weeks pregnant - who responded to me on Facebook - and said that they could fit us in. So, we made an appointment with Birth Options Midwifery for the following day (38 weeks +1 day).
Additionally, to determine if we were making the right decision, we thought we would still feel comfortable sticking with our OBGYN’s appointment for the following day as well, as long as we could get something in writing from the doctor. We sent the following email:
“I hope you had a good weekend. Would you be able to send copies of medical records from all our visits with Dr. XXXX, including the most recent one last Thursday?
In our last appointment with Dr. XXXX, she did mention that we needed to sign the consent forms and have them sent back or we would need to look for a different OBGYN. We did sign them and send them back in the last email, but would it be possible for us to sign a separate release form stating we decline certain procedures and understand the risks involved declining the procedures instead? I've done more research about the benefits and risks regarding labor and delivery procedures and don't feel comfortable with signing off on consent for them. For example, I decline any type of induction before week 42, all assisted delivery unless life-threatening emergency, and any episiotomy (unless preeclampsia - which is not an issue for us currently). Additionally I decline manual removal of placenta unless it is a retained placenta, and decline the epidural. We would like a natural birth. If it is possible to sign a paper releasing Dr. XXXX from liability caused by our birth preferences, we would like to have it ready for us to sign at our appointment tomorrow morning. (Please see our attached updated birth preferences document).
Alternatively, if this is not possible, please cancel our appointment for tomorrow morning. Either way, we would like to have the medical records from all our previous appointments for our records. Thank you.”
We received an email response simply stating:
“Dr XXXX has asked that I request that you please keep the appointment tomorrow at 10h00 so that she can have a frank discussion with you. She will also do a check-up and ultrasound at the meeting. After this discussion you can decide on the way forward.”
No forms or medical records were attached, so we abruptly canceled the appointment and let them know that they would be hearing from us in the near future. We were now pretty much with “Birth Options Midwifery” but we hadn’t even had our first consultation yet, so we couldn’t really “cancel” our OBGYN or Mediclinic until after we had another doctor/team and hospital situated.
Here’s some info on Birth Options Midwifery that we pulled from their website:
Our first appointment with Birth Options was pretty amazing, with Susan. She didn’t use those fancy machines with the monitors where you can “see your baby” like they used at the OBGYN’s office. BUT, something even better, she had us both feel around on Jenny’s belly for specific things “What you feel right here is a foot, and over here is his back, and shoulders, and this is his head”. It was much more personal and we felt 10 times better after that appointment than we felt at any appointment with the prior OBGYN’s. We were so glad that we had come here… and we were basically instant clients after that.
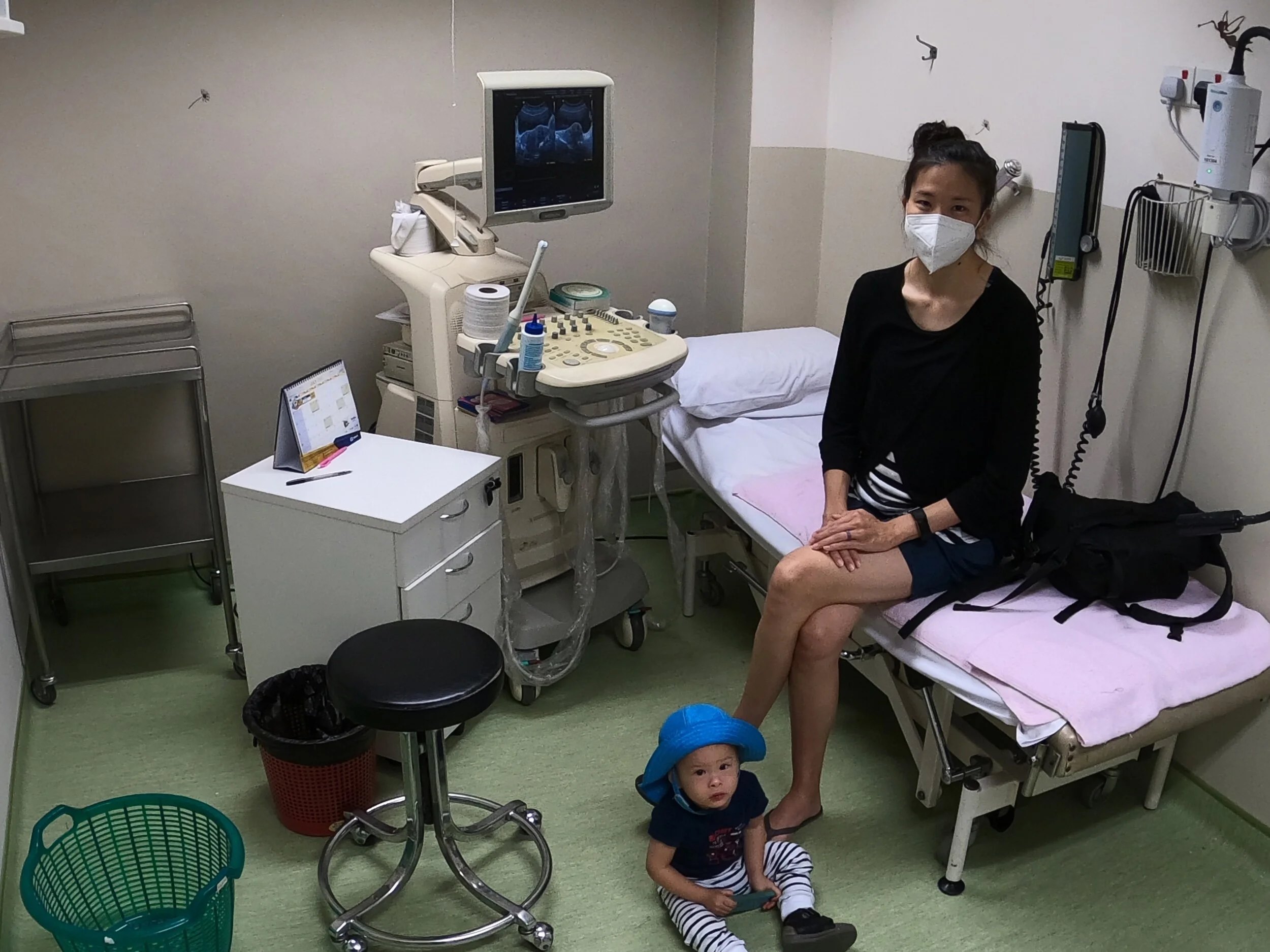
They also informed us that it is the law that the OBGYN has to give us our records if we request them, so they requested them on our behalf and attained them. After they read them over, they asked us to schedule an appointment with a Sonographer at Fetal View to have a Growth Scan, because the notes that were sent to Birth Options from our OBGYN stated that our baby was in the bottom range for abdominal circumference - as noted earlier - and that it might be an issue to get a new OBGYN (that they use as a back-up in case of emergencies) if the baby seemed risky.
We went to the Sonographer at 38 weeks +3 days and the exam showed that growth was very normal and that the baby was properly positioned to come out any day now. Plus, as it turns out, the Sonographer that we had at Fetal View was one that worked with Origin Maternity Hospital (our First Hospital). Very interesting!
That same day we had another appointment with our potential new “back-up” OBGYN at Melomed Private Hospital. She had received the new scans from Fetal View before we arrived and after filling out a bit of paperwork, we had a new OBGYN - Dr. Hendricks! Additionally, we were then able to pre-register for birth at Melomed and therefore could also cancel our reservations with the previous OBGYN and Hospital. Refunds from those two, after having made payment with a credit card (we used one for “points”), were quite difficult to figure out as both places preferred to do refunds to our bank accounts - but what they meant was “South African bank account”, and we didn’t have a bank account in South Africa! However, we did end up getting our refunds eventually.
At 39 weeks +1 day we had our second appointment with Birth Options and 40 weeks +1 day we had our third appointment with Birth Options. Both went very well - but now we were over 40 weeks, something our previous OBGYN wouldn’t have allowed. So, we also got Jenny a “Pregnancy Massage” on that same day with Vaunda. Jenny says that it was a much needed massage and definitely helped her feel better. However, it didn’t end up helping put her into labor (haha)!
As a side note, we were getting quite worried because it was now February 6th, and our 90-day visas were set to expire on March 2nd. Our time was running out to get things done, especially the important things like getting a Birth Certificate from Home Affairs and getting a Passport from the Consulate General of the United States.
Jenny’s parents arrived the following day, and we had a number of plans for them to see what Cape Town was all about. So, we spent the next 4 days exploring Cape Town while over 40 weeks pregnant. At 40 weeks +6 days, we went to Kirstenbosch National Botanical Garden and hiked up some of the hills to get some great views. The hiking definitely helped.
The following day, at 41 weeks, very early in the morning - slightly after midnight, Jenny began having contractions. We followed the recommendations in the “Natural Childbirth the Bradley Way” book and waited until all the signs were showing and then we headed to the hospital. They recommend waiting until the right time so that you aren’t stuck spending all day at the hospital, because hospitals tend to like to induce women who are there too long (3 hours or so) and we didn’t want to have that happen to us.
We got Jenny to a labor room and I ran down to get the bags. When I got back up, Bernice came in and started asking Jenny some questions. I was told to go downstairs to sign us in as patients at the hospital. I had only just sat down and started answering questions when a nurse informed me that I had to be upstairs because Jenny was already beginning to push! I ran upstairs as quickly as I could and made it there just in time… to experience 75 minutes of pushing!
However, it seemed that Jenny began this stage so quickly that Bernice didn’t have time to set anything up. We didn’t have the birth stool, the floor mats, the large rubber ball, the water tub, or anything like that. Bernice did have Jenny try a few different positions - kneeling on the bed while leaning forward and resting her arms and head on the elevated head-side of the bed, then squatting on the floor with me holding her up from behind while I was seated on a chair, and lastly just laying on her back on the bed. We might have tried a few more positions, but Jenny was already starting to breach, so it didn’t make sense to move her into any different positions at that time. This position lasted for roughly half of the 75 minutes of pushing, and Bernice was getting worried. Jenny was getting very exhausted with so much pushing, so Bernice recommended that we make a small cut. Eventually, we agreed and a small cut was made - after which our son came out immediately.
The cord turned white within a minute and was hence cut as all the blood had been delivered to our newborn son, and a little while later - with a slight bit of physical assistance from Bernice - the placenta was also birthed. Bernice sewed up the cut that was made and we were left to spend an hour with our son - skin-to-skin - while Bernice cleaned up the room. We were then moved to our regular room.
Jenny did have some issues feeling really nauseated afterward, but we were explained that this was likely exhaustion. After Bernice left, Jenny also had an issue with bleeding where she fainted in the restroom (while nurses were present - so they took care of her). As it turns out, the same thing (fainting) happened to her sister a few years prior during the birth of her first son. Either way, Jenny was looking very pale and I was quite a bit concerned with her health. However, our “back-up” OBGYN did come in to check her out and ended up giving her some medication to help contract her uterus as well as an intravenous bag (IV) with liquids. I got her some juices to drink and tried to get her to eat as much food as I could. The pediatrician came by to take a look at the baby - and noticed Jenny’s pale color as well. After that, Jenny took a nice long nap while I watched over our son - with the help of Jenny’s parents of course!
Later in the evening we had to hire an Uber to drive Jenny’s parents back to their accommodations as I would be staying the night at the hospital. Jenny had more to eat and drink before going to sleep.
By the next morning she was looking much better. Angela, a different one of the 4 midwives, came by to check on us and the baby and to give us any needed further instructions. The pediatrician also came by to do another check and asked the nurse to take a vial of blood to check for jaundice. I thought it was just going to be a small skin prick (similar to a diabetes test) and didn’t realize it would be a full sized baby-vial of blood. Our little boy screamed the whole time she squeezed his foot to have it bleed into the vial - it was quite difficult for me to bear as it lasted for nearly 3-4 minutes, but we got it over with eventually. As a side note: this was only an introduction to the screaming we would be hearing over the next couple of months (the joys of parenthood! haha).
Jenny ate her breakfast and her spirits were up. She was no longer looking pale, so we decided that we would attempt to check out of the hospital just after noon.
After we were all packed up, the hospital was kind and brought us both some lunch, with non-alcoholic champagne (sparkling grape juice) that really made it special. Then we checked out and headed home. What an experience! We have a son! We are now “Mommy & Daddy!”
As a personal note, we would like to thank the team at Birth Options Midwifery, they were definitely the best option in Cape Town for a natural delivery. (Note from Jenny: The Bradley Method book definitely helped prepare us for labor and delivery as I was able to labor mostly at home and was 9 cm dilated by the time we got to the hospital. I should have drank more fluids and maybe ate some food though as I was exhausted by the time I needed to push. So while the episiotomy may have been avoided at the end had we stuck strictly to the Bradley Method, I didn’t have much energy left in me and was open to having the cut to speed up the delivery.)
*** As US Citizens, our Visa-on-Arrival was 90 days long. Thus, we arranged to arrive roughly around month 7. Some airlines require a medical note to fly at 7-months, but it was not an issue for Jenny as she wasn’t showing much at that time. We even found time to do a number of day tours in Cape Town and go on a Garden Route Tour as well as a couple Private Game Reserve Safari’s! It was an amazing adventure!
If you are set on having a Bradley Method trained Midwife - and a birth in South Africa - we did notice one in the Johannesburg area, but we couldn’t find one in Cape Town.
Additionally, even though our son was born a week ‘late’ according to the due date that we were given, we would like to note that the “due date” is a completely ambiguous number and should NEVER be used as a definite deadline. They can be off by as much as 2 FULL weeks! Even in the past, Full-Term was defined as “between 37 and 42 weeks” (see “HealthLinkBC”). Doctors now differentiate between Early-Term, Full-Term, Late-Term, and Post-Term (see The Bump article: “How Doctors Now Define Full-Term Pregnancy”). Only “Post-Term”, which is defined as “after 42 full weeks of pregnancy”, is still considered “overdue”. Additionally, after looking back at our records, the longest that our son could have possibly been in-utero was 40 weeks +1 day, not 41 weeks (according to the start of the last period). So, if we had allowed induction at 39 weeks - it is likely that the baby would have technically been born “Early Term” - which is worse than Late-Term, according to The Bump.
In the end, we were still able to get a birth certificate from Home Affairs, and an Emergency Passport from the Consulate in time for our departure to Thailand. At just 16 days old, our son had his first, second, and third flights - to Johannesburg, Hong Kong, and then Bangkok, Thailand! You can catch up on where we are at now by checking out Our Blog or Instagram channel!
Please check out some of our other amazing tips on traveling while pregnant and traveling with a baby (like what baby travel gear we have found most useful or too cumbersome) in our Traveling for Parents section.
Thank you VERY much for reading our article. We actually created this website to help people reach financial independence. Did you know that by having a remote job and traveling endlessly, or living in a country that has low costs of living, you can actually reach retirement quicker? Plus, retirement abroad is up to 75 percent cheaper as well! Learn more by exploring our website: EatWanderExplore and REmotiFIRE.
See our Thank You page to sign up for our free weekly newsletter - you’ll receive only 1 email per week letting you know about our latest travel articles, remote-work life, and amazingly affordable destinations!
Found this post useful? Buy us a coffee to help support this site’s running costs OR share this article with a friend.